10 Powerful Reasons Why PPRN Networks Transform Patient Research
For many people, research once felt distant and abstract. Doctors and scientists made decisions. Patients simply received them. Today, that model is changing fast. At the heart of this change is a new idea: patient-powered research networks, often called PPRN networks.
Instead of being passive subjects, patients now help decide what questions matter. They share data, set priorities, and even sit on steering committees. This shift aligns closely with the vision of the Patient-Centered Outcomes Research Institute (PCORI) and the national PCORnet initiative. Together, they are reshaping how we study real-life health care. 🧬
Below are 10 powerful reasons why these networks transform patient research, and why this matters to you, your family, and your care team.
1. PCORI Puts Patients at the Center of Every Study
PCORI is an independent, non-profit organization created under the Affordable Care Act in 2010. Its mission is simple but ambitious. It wants patients, caregivers, and clinicians to have the evidence they need for informed choices.
PCORI focuses on patient-centered outcomes. That means:
- Asking which treatments help people live the lives they value
- Looking beyond lab results to daily function and quality of life
- Supporting research that patients help design and interpret
PCORI funds projects across five national priority areas:
- How we prevent, diagnose, and treat conditions
- How to improve healthcare systems
- How to communicate and share findings
- How to reduce disparities in care
- How to advance methods for patient-centered research
Patient-powered networks grow directly from this mission. They turn high-level goals into daily collaboration between patients, researchers, and health systems. 🤝
2. PPRN Communities Give Patients Real Power in Research Decisions
Within PCORnet, one entire pillar is built around PPRN communities that patients lead. These are not small focus groups. Ideal networks often aim for 50,000 or more members, except in rare diseases.
In these networks:
- Patients help define which questions deserve funding
- They co-create study protocols and consent processes
- They sit on steering committees and advisory boards
- They help review results before publication
This structure gives patients real governance power. Leaders work to ensure diversity across age, race, geography, and health status. That diversity makes findings more representative of real communities, not just one narrow group.
For example, a network for people with chronic pain might vote to prioritize safe long-term medication strategies over very rare experimental procedures. That choice comes from lived experience, not only academic interest.
3. Data Sharing Becomes Easier, Safer, and More Patient-Controlled
A key strength of patient-powered research networks is data. Each network builds a standards-based infrastructure designed for safe sharing.
Patients are encouraged to:
- Share electronic clinical data from hospitals or clinics
- Use tools such as Blue Button to download health records
- Report their own symptoms, side effects, and daily outcomes
Because networks use interoperable standards, data from different clinics and systems can be combined. This allows researchers to:
- Compare treatments across large, diverse populations
- Study long-term outcomes, not just short-term changes
- Spot patterns that single clinics might miss 📊
At the same time, governance structures keep patients in control. Transparent policies explain:
- What data are collected
- How they will be protected
- How they will be used and shared
Many networks allow patients to adjust preferences. They can choose which studies to join or which data elements to share.

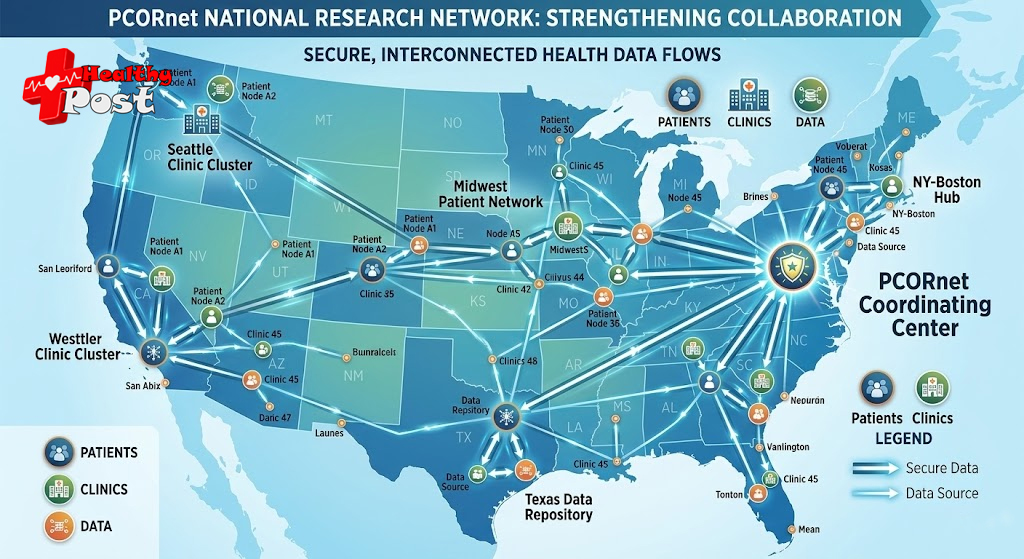
4. PCORnet Connects PPRN Groups With Health Systems Nationwide
PCORI created the National Patient-Centered Clinical Research Network (PCORnet) to expand comparative effectiveness research. PCORnet has three main parts:
- Clinical Data Research Networks (CDRNs)
Hospital and health-system networks that hold clinical records. - Patient-Powered Research Networks
Patient-led groups organized around shared conditions or experiences. - A Coordinating Center
Provides technical, methodological, and logistical support.
This structure lets patient-led groups connect with major health systems. Data can flow, under strict safeguards, between patient communities and hospital records.
That connection allows:
- Faster recruitment into studies
- Access to clinical lab and imaging results
- Richer, more complete outcome tracking
Patients bring their priorities. Health systems bring detailed medical data. Together, they enable real-world comparative effectiveness research at national scale.
5. Networks Can Address Everyday Conditions, From Heart Disease to Tooth Enamel Erosion
One of the strengths of these networks is their flexibility. They can focus on many conditions, from common to rare. That includes topics that matter deeply to quality of life, such as oral health. 🦷
Consider people worried about tooth enamel erosion stages. Many wonder:
- Which drinks or habits speed up the damage?
- Which approaches work best for fixing tooth enamel erosion?
- What is the safest tooth enamel erosion treatment over many years?
- Is there evidence on how to restore tooth enamel naturally?
A patient-powered network focused on oral health could:
- Collect daily reports on diet, brushing habits, and pain
- Combine them with dentist records and photos
- Compare different treatments and self-care strategies
- Share results in clear, patient-friendly language
This kind of study may be overlooked in traditional academic settings. Yet it can strongly affect comfort, confidence, and social life. Patient-led priority setting ensures such concerns do not stay invisible.
6. Meaningful Use and Blue Button Tools Unlock Rich Clinical Information
To build strong networks, PCORI encouraged groups to tap into existing federal initiatives. Two especially important ones are Meaningful Use of electronic health records and the Blue Button feature.
These efforts make it easier for patients to:
- Access digital copies of their health information
- Share that information with trusted networks
- Track health changes over time
Within a patient-powered research network, these tools support:
- Automated collection of lab values and diagnoses
- Reduced manual data entry for patients and staff
- Quicker identification of people eligible for certain studies
For example, a network focused on diabetes could identify:
- People with high A1c levels from clinic data
- Patients reporting fatigue and burnout in surveys
- Patterns linking treatments, behaviors, and outcomes
The result is more accurate, timely, and less burdensome research.
7. Early Funding Focused on Building Strong Foundations, Not Quick Trials
PCORI’s early funding for patient-powered research networks was infrastructure-focused. The 18‑month initiative supported up to 18 networks, with a total budget of $12 million.
Key goals included:
- Recruiting robust patient membership
- Building technical data platforms using shared standards
- Describing who belongs to each network
- Identifying research topics patients most want addressed
- Collecting both clinical and patient-generated data
Importantly, this was not about running many clinical trials immediately. Instead, it created:
- Trusting patient communities
- Reliable data systems
- Governance models that respect patient authority
These foundations now allow future studies to launch more quickly and responsibly.
8. Transparent Governance Builds Trust and Representation
Trust is essential in any research relationship. Patient-powered networks address this through clear governance and patient control.
Strong networks:
- Involve patients in leadership, not just consultation
- Document how decisions are made
- Commit to reporting findings back to members
- Actively recruit underrepresented communities
Governance frameworks help answer questions like:
- How will data be de-identified and protected?
- Who reviews study proposals and why?
- How are conflicts of interest managed?
- How will results be shared with participants and the public?
These structures reduce the risk of tokenism. Patients are not there for appearance only. They share real power and responsibility.
You can read more about PCORI’s approach to governance and priorities in an official according to article/topic from PCORI at
https://www.pcori.org
9. Methodologic Innovation and Collaboration Raise Research Quality
PCORI’s national priorities include accelerating patient-centered outcomes research and methods. Patient-powered networks are a testbed for that mission.
Because they connect many sites and community groups, they can:
- Compare different ways of collecting patient-reported outcomes
- Test new approaches to informed consent
- Explore best practices for engaging underrepresented groups
- Improve ways to communicate results clearly
Many networks plan to merge or connect with Clinical Data Research Networks in later cycles. This deepens collaboration between community groups and large health systems.
Researchers also receive support from a national Coordinating Center. This hub shares:
- Statistical tools
- Data standards
- Study design guidance
- Ethical frameworks for patient engagement
Together, these features improve both the rigor and the relevance of studies.
You can explore how PCORnet operates within this broader framework in an informative according to article/topic from PCORnet at
https://pcornet.org
10. Long-Term, These Networks Help Patients and Clinicians Make Better Choices
Ultimately, the aim of all this effort is simple. People should have evidence that reflects their realities and goals. That includes patients, families, clinicians, policymakers, and payers. 💡
When patient-powered networks function well, they can:
- Answer everyday questions faster and more clearly
- Reduce wasteful or ineffective treatments
- Highlight which approaches work best for which people
- Support shared decision-making in the clinic
- Reveal and reduce disparities in care access or outcomes
Imagine a parent choosing between two asthma treatments for a child. Or an older adult deciding whether to start a new heart medication. Or someone comparing options for tooth enamel erosion treatment while balancing cost and comfort.
Evidence from large, inclusive networks can guide these decisions. It helps ensure care is not just technically correct, but also aligned with what people value most.
Quick Comparison: Components of PCORnet
| Component Type | Who Leads It | Main Data Sources | Key Strength |
|---|---|---|---|
| Clinical Data Research Networks (CDRNs) | Health systems, hospitals, clinics | Electronic health records, labs, procedures | Large clinical datasets from real-world care |
| Patient-Powered Research Networks | Patients and caregivers | Patient-reported outcomes, shared clinical data | Strong patient voice and lived experience |
| Coordinating Center | National research and informatics experts | Metadata from all networks, methods resources | Standardization, support, and quality control |
FAQs About Patient-Powered Research Networks
1. What is a patient-powered research network?
It is a research community led by patients and caregivers. Members help set priorities, share data, and guide studies that reflect their lived experiences.
2. How is a PPRN different from a traditional research registry?
Traditional registries mostly collect data from patients. A patient-powered network goes further. Patients share leadership, shape questions, and influence how findings are shared.
3. Who can join these networks?
Most networks welcome people living with a condition, caregivers, clinicians, and sometimes healthy volunteers. Eligibility varies by network focus and goals.
4. How does PCORI ensure studies are safe and ethical?
Studies funded by PCORI follow strict ethical rules. Independent review boards, transparency about risks, and patient governance structures all help protect participants.
5. Do PPRN networks replace clinical trials?
No. They complement clinical trials. Networks help identify key questions, recruit participants, and follow people long term. Many trials now build on these infrastructures.
6. Are these opportunities only for large diseases?
No. Smaller patient-powered networks support rare diseases too. Membership targets adjust for disease prevalence, while still aiming for strong representation.
Conclusion: How PPRN Networks Are Redefining Patient-Centered Research
Patient-powered research networks show what happens when patients move from the sidelines to the center of research. They embody PCORI’s mission and bring PCORnet’s vision to life.
Through shared data, thoughtful governance, and real collaboration, these communities help answer the questions people actually ask in daily life. Whether someone is managing diabetes, heart disease, or worrying about how to restore tooth enamel naturally, they deserve clear, relevant evidence.
As more clinicians, health systems, and patients engage, the influence of the pprn model will continue to grow. If you belong to a community affected by a specific condition, consider joining or supporting a patient-powered network. Your story and your data can help shape better care for everyone. 🌟