
Tooth Enamel Erosion Causes: 7 Shocking Stages & Treatments You Must Avoid
If your teeth feel more sensitive than they used to, you are not alone. Many people struggle with damage from everyday habits without realizing it. Understanding tooth enamel erosion causes can help you protect your smile before the problem becomes permanent.
You do not need a dental degree to follow this guide. We will walk through the real tooth enamel erosion stages, the risky “treatments” to avoid, and safer steps you can take instead. Think of this as a supportive roadmap, not a lecture.
By the end, you will know what might be harming your enamel, what warning signs to watch for, and how to work with your dentist to slow or stop further damage.
What Is Tooth Enamel and Why Does It Matter?
Enamel is the thin, hard outer shell of your teeth. It protects the softer layers underneath from hot, cold, chewing, and bacteria.
Once enamel is worn away, it does not grow back like skin or nails. That is why prevention and early action are essential.
Most tooth enamel erosion causes share one thing in common: acid. Acid can come from food, drinks, stomach reflux, or even dry mouth. Over time, that acid can dissolve minerals from the enamel surface.
7 Shocking Tooth Enamel Erosion Stages
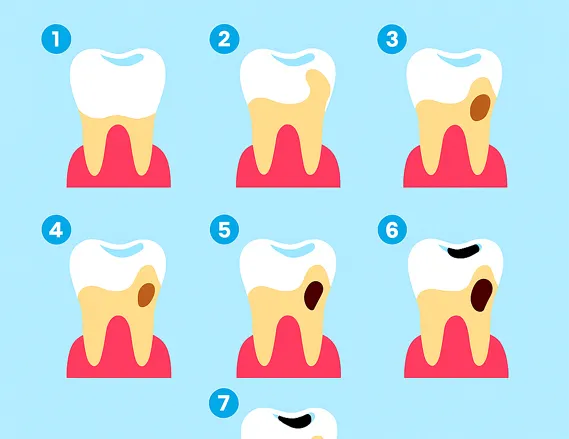
Tooth damage rarely happens overnight. It usually follows a pattern. Knowing these tooth enamel erosion stages can help you recognize trouble much earlier.
Stage 1: Early Softening You Cannot See
At first, enamel looks normal in the mirror. Under the surface, minerals are slowly dissolving after repeated acid exposure.
You might notice:
- Mild sensitivity to very sweet foods
- No visible holes or chips yet
Risky “treatment” to avoid:
- Brushing hard right after acidic drinks or vomiting. This scrubs softened enamel away.
Better steps:
- Rinse with plain water after acidic food or drinks.
- Wait at least 30 minutes before brushing.
Stage 2: Chalky White Spots and Dullness
Next, enamel starts to lose its natural shine. You may see flat, chalky white patches, especially near the gum line.
You might notice:
- Teeth look less glossy and more matte
- Increased sensitivity to cold air or drinks
Risky “treatment” to avoid:
- DIY whitening pastes with lemon juice or vinegar. These are extremely acidic.
Better steps:
- Switch to a fluoride toothpaste for sensitive teeth.
- Ask your dentist about professional fluoride varnish or remineralizing gels.
Stage 3: Thinning Enamel and Shape Changes
As erosion continues, the teeth can actually change shape. Edges may look more translucent, thin, or irregular.
You might notice:
- Front teeth edges look see-through or glassy
- Molars develop shallow, smooth “dents” or cups
- Teeth seem shorter than before
Risky “treatment” to avoid:
- Unsupervised orthodontic aligners bought online. Moving already weak teeth can increase chipping risk.
Better steps:
- Get a full dental exam and photos to track changes.
- Ask about custom trays for safe, dentist-guided whitening if needed.
Stage 4: Sensitive Yellow Dentin Showing Through
Below enamel lies dentin, which has a yellowish color. When enamel thins enough, teeth start to appear more yellow.
You might notice:
- Ongoing sensitivity to hot and cold
- Yellow areas that do not improve with whitening
- Food and drinks triggering “electric” twinges
Risky “treatment” to avoid:
- Aggressive whitening strips or gels. They can worsen sensitivity and do not fix the real problem.
Better steps:
- Work with your dentist on a careful tooth enamel erosion treatment plan.
- Use desensitizing toothpaste daily and reduce acidic exposures.
Stage 5: Small Chips, Cracks, and Uneven Edges
Weakened enamel is more likely to chip or crack. Even normal biting pressure can cause small breaks.
You might notice:
- Sharp edges that catch your tongue
- Small chips on front teeth
- Cracks or lines that trap stain
Risky “treatment” to avoid:
- At-home filing or reshaping trends seen on social media.
- Biting on pen caps, ice, or hard candies.
Better steps:
- Ask about bonding to smooth and protect chipped areas.
- Wear a night guard if you clench or grind your teeth.
Stage 6: Deep Wear and Flattened Biting Surfaces
At this point, much of the protective layer is gone on some teeth. Biting surfaces look flat, shiny, and worn down.
You might notice:
- Difficulty chewing certain foods comfortably
- Jaw fatigue or soreness from altered bite
- Frequent sensitivity in several teeth at once
Risky “treatment” to avoid:
- Cheap mail-order veneers or crowns without in-person evaluation.
Better steps:
- Consult a dentist experienced in fixing tooth enamel erosion and bite problems.
- Discuss options like onlays, crowns, or protective overlays.
Stage 7: Severe Erosion, Exposed Nerves, and Tooth Loss Risk
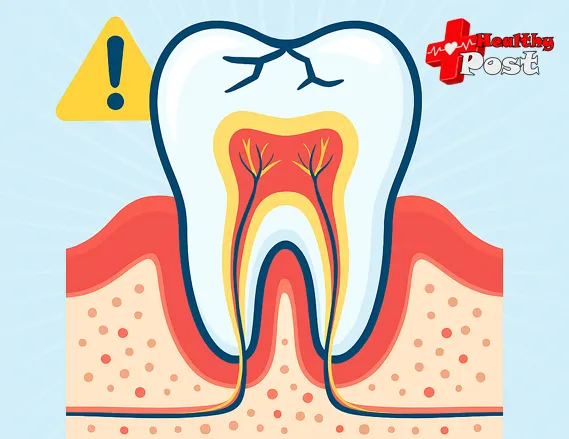
In the final stage, inner layers may be exposed. Pain can be severe, and infection risk is much higher.
You might notice:
- Spontaneous tooth pain without an obvious trigger
- Very sharp sensitivity that lingers
- Broken teeth or teeth worn nearly to the gum line
Risky “treatment” to avoid:
- Delaying care and relying on painkillers only.
- Unregulated “miracle” solutions that promise to regrow enamel completely.
Better steps:
- Seek urgent professional care. You may need root canals, crowns, or extractions.
- Work with your dentist and doctor to address underlying medical causes.
Common Tooth Enamel Erosion Causes You Might Miss
Many tooth enamel erosion causes hide in everyday routines. Some feel harmless, even healthy, until damage appears.
Acidic Drinks and Foods
Acidic items soften enamel, especially with frequent sipping or snacking.
- Soft drinks, including diet sodas
- Energy and sports drinks
- Citrus juices, kombucha, vinegar drinks
- Frequent sucking on lemons or sour candies
Helpful habits:
- Drink water with or after acidic drinks.
- Use a straw to reduce direct contact when possible.
- Keep acidic treats to mealtimes, not all day.
Frequent Snacking and Grazing
Every time you eat, mouth bacteria produce acid for a while. Constant grazing means almost constant acid.
Helpful habits:
- Leave gaps between snacks so saliva can neutralize acids.
- Choose cheese, nuts, or vegetables instead of sugary snacks.
Stomach Acid Reflux and Vomiting
With reflux, stomach acid travels upward, bathing back teeth in very strong acid. Regular vomiting has a similar effect.
This is common with:
- Chronic reflux disease (GERD)
- Eating disorders
- Pregnancy-related nausea
- Certain medications or surgeries
Helpful habits:
- Rinse with water or a baking soda solution after reflux or vomiting.
- Avoid brushing for at least 30 minutes afterward.
- Work with your doctor to manage the medical cause.
Dry Mouth (Xerostomia)
Saliva protects enamel by washing away food and neutralizing acid. When you have dry mouth, acid damage increases.
Common causes include:
- Many blood pressure, allergy, and mood medications
- Autoimmune conditions such as Sjögren’s syndrome
- Smoking or vaping
- Dehydration and mouth breathing
Helpful habits:
- Drink water regularly throughout the day.
- Chew sugar-free gum with xylitol to stimulate saliva.
- Ask your dentist about saliva substitutes or gels.
Overbrushing and Abrasive Toothpastes
Brushing too hard, especially with a hard-bristled brush, can wear enamel away. Abrasive whitening pastes can also contribute.
Helpful habits:
- Use a soft brush and gentle, small circles.
- Let the toothpaste and time do the work, not pressure.
- Limit aggressive whitening pastes if you have sensitivity.
Teeth Grinding and Clenching
Grinding, also called bruxism, can wear enamel faster than chewing alone. It often happens at night without awareness.
Helpful habits:
- Ask a dentist if you need a night guard.
- Practice stress management and jaw relaxation techniques.
Safe Approaches for Fixing Tooth Enamel Erosion
You cannot magically regrow lost enamel, but you can slow damage and strengthen what remains. Fixing tooth enamel erosion usually means combining home care with professional treatment.
Remineralizing Early Damage
In early stages, minerals can be added back into softened areas. This helps enamel become harder again.
Options may include:
- Fluoride toothpaste and mouth rinses
- Professional fluoride varnish at checkups
- Products containing calcium and phosphate compounds
This approach works best before deep cavities form. Routine dental visits make early detection easier.
Professional Tooth Enamel Erosion Treatment
Dentists tailor treatment to your erosion stage, symptoms, and bite. There is no single solution for everyone.
Possible treatments include:
- Bonding with tooth-colored resin for chips and worn edges
- Inlays, onlays, or crowns to rebuild height and strength
- Night guards to shield teeth from grinding
- Coordinated care with doctors for reflux or dry mouth
If you feel nervous about treatment, share that with your dentist. A supportive team will explain options clearly and respect your pace.
How to Restore Tooth Enamel Naturally (What That Really Means)
Many people search for how to restore tooth enamel naturally. It is important to be clear: you cannot grow entirely new enamel at home.
However, you can:
- Support remineralization of softened enamel areas
- Protect remaining enamel from further acid attacks
- Improve saliva flow and tooth-friendly nutrition
Gentle, helpful habits include:
- Drinking plenty of water instead of sugary or acidic drinks
- Eating dairy, leafy greens, nuts, and other mineral-rich foods
- Using fluoride toothpaste twice daily
- Chewing sugar-free gum with xylitol after meals
Be skeptical of any product that claims to rebuild enamel completely. Your dentist is your best guide for safe options.
Treatments and Trends You Must Avoid
Some popular trends can quietly speed up tooth erosion. Understanding these risks can save you pain, money, and stress.
Overuse of DIY Whitening Remedies
Many home whitening recipes use strong acids or harsh abrasives. These might lighten stains but harm enamel at the same time.
Risky ingredients include:
- Lemon juice or other citrus juices
- Vinegar, including apple cider vinegar
- Baking soda used aggressively and often
- Hydrogen peroxide left on teeth for long periods
Safer choice:
- Ask your dentist about supervised whitening options.
- Use products with the ADA Seal or your country’s equivalent label.
Charcoal and Abrasive Powders
Charcoal toothpastes and powders are trendy. Many are very abrasive and can scratch enamel surface over time.
Scratched enamel holds stains and plaque more easily. It also appears dull and worn.
Safer choice:
- Use non-abrasive toothpaste labeled as gentle or enamel-safe.
- Focus on thorough but gentle brushing technique.
Unsupervised Online Orthodontic and Cosmetic Kits
Aligners, veneers, and bonding kits sold online promise quick results. Without a full exam, they may be used on already damaged teeth.
Results can include:
- Worsened bite and jaw pain
- Chips or fractures of thin enamel
- Trapped decay under poorly fitted coverings
Safer choice:
- See a local dentist or orthodontist for a full evaluation.
- Discuss both appearance goals and enamel protection.
Ignoring Medical and Lifestyle Roots of Erosion
Reflux, eating disorders, medication side effects, and dry mouth are not “just dental problems.” They affect your whole health.
Avoid:
- Blaming brushing alone when symptoms continue to worsen.
- Hiding symptoms from your dentist out of embarrassment.
Safer choice:
- Share your full medical and lifestyle history with your dentist.
- Ask about referrals to doctors, dietitians, or counselors if needed.
Quick Reference: Tooth Enamel Erosion Stages and Safe Actions
| Stage | What You May See or Feel | Risky “Treatments” to Avoid | Safer Actions to Consider |
|---|---|---|---|
| 1. Early Softening | Mild sensitivity, no visible changes | Brushing hard after acid exposure | Rinse with water, wait to brush |
| 2. Chalky Spots | White, dull patches on enamel | Lemon or vinegar whitening mixes | Fluoride toothpaste, dental checkup |
| 3. Thinning Enamel | Translucent edges, shallow dents | Unsupervised aligner treatments | Professional exam, custom plan |
| 4. Yellow Dentin Showing | Yellow tone, strong sensitivity | Aggressive at-home whitening | Desensitizing toothpaste, dentist-guided care |
| 5. Chips and Cracks | Sharp edges, small chips | DIY filing or reshaping | Bonding, night guard if grinding |
| 6. Deep Wear | Flat, worn biting surfaces | Cheap mail-order veneers or crowns | Onlays, crowns, bite adjustment |
| 7. Severe Erosion | Major pain, broken teeth | Delaying treatment, miracle “regrowth” claims | Urgent dental care, medical support |
Frequently Asked Questions About Enamel Erosion
Can enamel erosion be reversed?
Early softening of enamel can sometimes be remineralized. Fluoride, saliva, and good habits help minerals return to the surface.
Once enamel is deeply worn or missing, it cannot grow back. At that point, dentists use bonding, fillings, or crowns to protect teeth.
How do I know if my enamel is eroding?
Common signs include increasing sensitivity, yellowing that does not respond to whitening, and changes in tooth shape. You might see flattened biting surfaces or small cups on molars.
A dentist can confirm enamel loss using light, X-rays, and photos. Regular checkups are the best way to catch changes early.
Is it possible to stop enamel erosion without dental treatment?
You can slow or reduce mild erosion by changing habits. This includes reducing acidic drinks, improving brushing technique, and supporting saliva flow.
However, established damage still needs professional evaluation. Without that, you risk cavities, fractures, and pain in the future.
What is the safest way to whiten my teeth if I have enamel erosion?
First, focus on stabilizing the erosion with your dentist. That might include desensitizing products and fluoride treatments.
Then ask about gentle, supervised whitening. Your dentist can choose products and timing that respect your enamel limits.
Can diet really help protect enamel?
Yes. A diet low in frequent sugar and acid supports enamel health. Mineral-rich foods and adequate water also help.
Dairy, leafy greens, nuts, and whole foods can support overall oral health. Combine this with consistent brushing, flossing, and dental visits.
Should I be worried about tooth enamel erosion in children?
Children’s enamel is thinner and more vulnerable. Frequent juice, soda, or sucking on citrus can cause early erosion.
Help children drink more water, limit sugary and acidic snacks, and see a dentist regularly. Early prevention sets them up for healthier adult teeth.
Conclusion: Take Control Before Enamel Erosion Goes Too Far
Tooth enamel erosion causes may feel hidden, but the effects are not. Sensitivity, yellowing, chips, and worn edges can affect comfort and confidence.
By understanding the tooth enamel erosion stages, you can act sooner and avoid risky “treatments” that might make things worse. Gentle habits, smart food and drink choices, and regular checkups go a long way.
If you recognize any signs described here, reach out to a dental professional. Ask about a personalized tooth enamel erosion treatment plan that fits your health, budget, and goals. Working together, you can protect the enamel you have, support remineralization where possible, and keep your smile comfortable for years to come.

2 thoughts on “Tooth Enamel Erosion Causes: 7 Shocking Stages & Treatments You Must Avoid”