7 Surprising Benefits of Laparoscopic Surgery: What Is It and How Scars Fade Fast
If you or someone you love has been told they may need laparoscopic surgery, it is normal to feel relieved and nervous at the same time. Surgery is still surgery. Yet this approach has changed the experience for millions of patients. Instead of one large incision, surgeons use a few tiny openings and a slim camera to work inside the body with far less disruption.
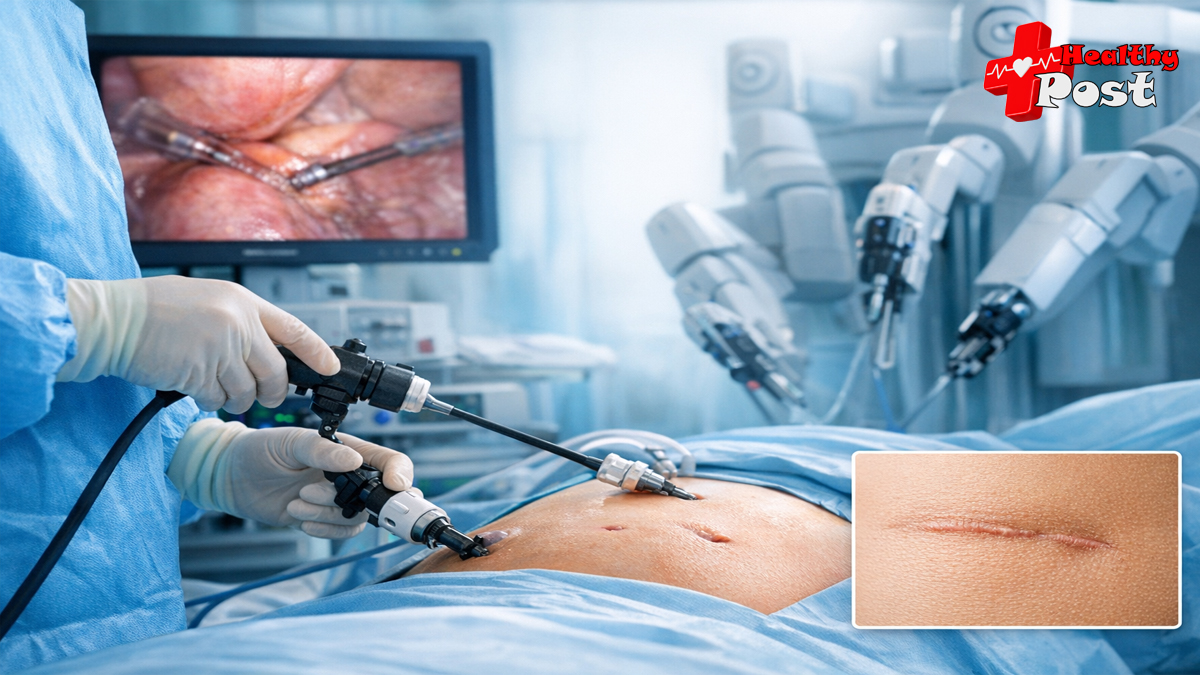
So, what is laparoscopic surgery in simple terms? It is a minimally invasive technique used to diagnose or treat problems in the abdomen or pelvis. A laparoscope, which is a thin tube with a camera, is placed through small incisions, often less than 1 centimeter. The surgeon watches a magnified image on a screen and uses delicate instruments to perform the procedure.
This method is now common for gallbladder removal, appendectomy, hernia repair, endometriosis treatment, bariatric procedures, and many gynecological surgeries. Beyond the medical side, many patients care about something deeply personal too: healing well and feeling comfortable in their body again. That is where the conversation around laparoscopic surgery scars becomes especially important.
In this guide, we will look at seven surprising benefits, explain the risks honestly, and show why scars often fade faster than people expect.
1. Smaller Incisions Mean Less Trauma to the Body
The first major benefit is visible from the start. Traditional open surgery often requires a long incision. Minimally invasive surgery usually uses two to four small cuts.
That difference matters more than it seems.
Smaller incisions often lead to:
- Less disruption of skin and muscle
- Less bleeding during surgery
- Lower strain on surrounding tissue
- A gentler healing process
Think of it like repairing a wall through a small access panel instead of tearing down half the room. The structure stays more intact.
For many procedures, these incisions are placed near the belly button or lower abdomen. Over time, they can become faint enough that people forget where they were. This is one reason many patients ask about laparoscopic surgery scars before they ask anything else.
Real-life example
A patient having gallbladder removal may go home with three or four tiny dressings instead of one long abdominal wound. That changes movement, comfort, and confidence during recovery.
2. Pain Is Often Lower Than With Open Surgery
Pain after surgery affects sleep, walking, breathing, and mood. It can also delay recovery if patients are afraid to move.
One reason laparoscopic surgery is preferred in many cases is that pain is often reduced. Since the incisions are smaller, the body has less tissue damage to repair. Many patients still feel soreness, bloating, or shoulder discomfort from the gas used during surgery, but this is often more manageable than pain from a large incision.
Lower pain can mean:
- Less need for strong pain medication
- Easier walking in the first day or two
- Better deep breathing and coughing
- Faster return to eating and sleeping normally
This matters especially for older adults and people trying to avoid prolonged opioid use.
According to the National Library of Medicine, minimally invasive approaches are widely studied for improved post-operative recovery and reduced surgical burden in many procedures.
3. Recovery Is Faster, Both Physically and Emotionally
This is the benefit patients remember most. Healing is not only about stitches. It is about getting back to ordinary life.
After laparoscopic surgery, many people resume light activity within 3 to 7 days, depending on the procedure. Full recovery still varies. A simple appendectomy is different from bariatric surgery or treatment for severe endometriosis. Still, compared with open surgery, the timeline is often shorter.
Here is how the two approaches usually compare:
| Factor | Laparoscopic Approach | Open Surgery |
|---|---|---|
| Incision size | Small, often under 1 cm | Larger abdominal incision |
| Hospital stay | Often shorter | Often longer |
| Pain level | Usually lower | Usually higher |
| Return to light activity | Often within days | Often takes longer |
| Scar appearance | Small, less noticeable | Larger, more visible |
| Infection risk | Typically lower | Typically higher |
The emotional impact is easy to underestimate. Smaller wounds can make patients feel less fragile. They may find it easier to shower, dress, and look at their body without distress.
That mental relief is real. For some, it becomes just as meaningful as the physical healing.

4. Scars Usually Fade Faster Than People Expect
Many people focus on whether surgery will “leave a mark.” The better question is how the mark will heal over time.
With laparoscopic surgery scars, the starting point is already smaller. Most incisions are short and placed in discreet areas. As swelling settles and skin remodels, scars often flatten and lighten over several months.
Why these scars tend to heal well
- The cuts are small
- Tension on the wound is lower
- There is less tissue injury
- Proper aftercare supports smoother healing
Tips to help scars fade well
- Keep incisions clean and dry
- Follow your surgeon’s instructions exactly
- Avoid heavy lifting too soon
- Protect healing skin from sun exposure
- Ask when scar gel or silicone sheets are safe to use
Not every scar heals the same way. Skin tone, genetics, age, smoking, diabetes, and infection risk all play a role. Some people develop darker marks or raised scars even after tiny incisions. But in general, cosmetic outcomes are favorable.
The American College of Surgeons offers patient education on surgical recovery and wound care that supports safe healing decisions.
5. The Risk of Infection and Blood Loss Is Often Lower
Every surgery carries risk. That should never be minimized. Still, one of the strongest advantages of this technique is that complications related to large wounds can be reduced.
When incisions are smaller, there is less exposed tissue. That can lower the chance of wound infection. Blood loss may also be less in many laparoscopic procedures, though the exact amount depends on the condition being treated and the patient’s health.
Possible benefits include:
- Lower wound infection risk
- Less blood loss during surgery
- Reduced need for prolonged hospitalization
- Lower chance of large-incision complications
This does not mean the procedure is risk-free. Complications can still include:
- Bleeding
- Infection
- Injury to nearby organs
- Blood clots
- Anesthesia-related problems
In some cases, the surgeon may need to convert to open surgery for safety. That is not a failure. It is a careful medical decision when visibility or access is limited.
If you are wondering what is laparoscopic surgery best suited for, the answer depends on your diagnosis, body history, prior surgeries, and overall health.
6. It Is Used for More Conditions Than Many People Realize
Some patients think this method is only for simple gallbladder or appendix problems. In reality, its reach is much broader.
Today, surgeons use laparoscopic surgery for many abdominal and pelvic conditions, including:
- Gallbladder removal
- Appendix removal
- Hernia repair
- Ovarian cyst surgery
- Fibroid treatment
- Ectopic pregnancy management
- Endometriosis diagnosis and treatment
- Bariatric procedures like gastric sleeve
- Some bowel procedures
This broad use has changed expectations in general surgery and gynecology. In many hospitals, minimally invasive surgery is now the standard option when medically appropriate.
A practical example
A woman with years of pelvic pain may undergo laparoscopy to diagnose and treat endometriosis at the same time. Instead of a large incision and a longer recovery, she may return to desk work much sooner.
For background on gynecologic uses and women’s health procedures, the ACOG provides trusted patient information that can help explain options clearly.
7. New Technology Is Making Results Even Better
The most surprising benefit may be what comes next. This field is still evolving.
From 2024 to 2026, several advances are improving outcomes:
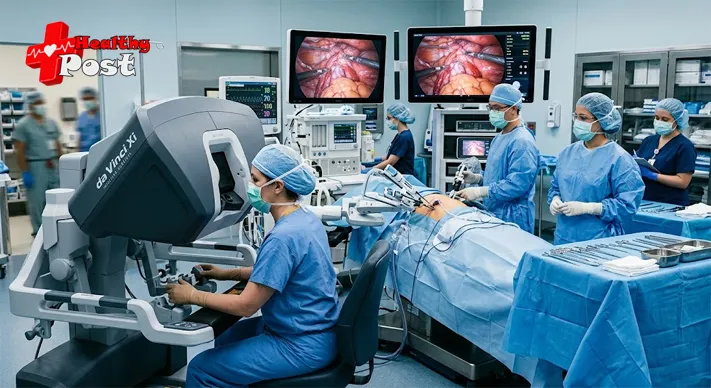
Robotic-assisted laparoscopy
Robotic systems help surgeons with precision, control, and visualization. The robot does not operate alone. The surgeon directs every movement. This can be useful in delicate pelvic and complex reconstructive procedures.
High-definition and 3D imaging
Modern imaging gives clearer views of anatomy. That can support safer dissection and better accuracy.
Natural orifice techniques such as vNOTES
Some gynecologic procedures now use access through natural openings, such as the vagina, reducing or even eliminating visible external scars.
Better outcomes in selected cases
Recent studies continue to show faster recovery and fewer complications in laparoscopic versus open approaches for several abdominal and gynecological conditions.
This also explains the rise of medical travel. Countries such as Turkey, India, and Thailand are increasingly known for minimally invasive surgical care, often at lower cost. For international patients, the appeal is not just price. It is expertise, shorter hospital stays, and faster return home.
It is a minimally invasive operation done through small cuts using a camera and special instruments.
Many people return to light activity in 3 to 7 days. Full recovery depends on the procedure.
Yes, but they are usually small and often fade significantly over time.
In many cases, it has lower infection risk, less pain, and faster recovery. Safety depends on the patient and procedure.
Yes. If access is limited or safety becomes a concern, surgeons may switch to open surgery.
🟢 CAPTION: “Robotic tools and advanced imaging are reshaping minimally invasive surgery.”
What to Know Before Choosing This Approach
It is not right for every patient.
Your surgeon may recommend against it if you have:
- Extensive scar tissue from prior operations
- Advanced cancer in some settings
- Severe bleeding disorders
- A condition that requires direct open access
A careful consultation matters. Ask:
- Am I a good candidate for minimally invasive surgery?
- What are the chances of converting to open surgery?
- How long will recovery take for my exact procedure?
- What should I expect from the scars?
- When can I return to work, exercise, and driving?
You may also want to read related articles using internal links such as recovery tips after abdominal surgery, signs your incision is healing normally, and questions to ask before elective surgery.
Frequently Asked Questions
1. What is laparoscopic surgery in simple words?
It is a minimally invasive operation done through small cuts using a camera and special instruments.
2. How long does it take to recover?
Many people return to light activity in 3 to 7 days. Full recovery depends on the procedure.
3. Are laparoscopic surgery scars permanent?
Yes, but they are usually small and often fade significantly over time.
4. Is it safer than open surgery?
In many cases, it has lower infection risk, less pain, and faster recovery. Safety depends on the patient and procedure.
5. Can laparoscopic surgery turn into open surgery?
Yes. If access is limited or safety becomes a concern, surgeons may switch to open surgery.
6. When should I call my doctor after surgery?
Call if you have fever, worsening redness, swelling, drainage, severe pain, or trouble breathing.
Conclusion
For many patients, laparoscopic surgery offers more than a technical upgrade. It offers a gentler path through a stressful experience. Smaller incisions, lower pain, shorter hospital stays, and faster recovery can make a major difference in daily life. And when it comes to laparoscopic surgery scars, the cosmetic outcome is often reassuring, especially with good aftercare.
Still, the best surgical plan is always personal. If you are considering this option, speak with a qualified surgeon about your diagnosis, your recovery goals, and whether a minimally invasive approach is right for you. A clear conversation today can make the entire journey feel more manageable tomorrow.
References
- National Library of Medicine — https://www.ncbi.nlm.nih.gov/
- American College of Surgeons — https://www.facs.org/
- American College of Obstetricians and Gynecologists — https://www.acog.org/
Dr. Sana Lodhi is a qualified medical doctor (MBBS) with a strong commitment to patient care and evidence‑based medicine. With years of clinical experience, she brings trusted medical insights to readers, simplifying complex health topics into clear, practical guidance. Her passion lies in promoting preventive healthcare, empowering individuals to make informed decisions, and bridging the gap between medical knowledge and everyday wellness. At HealthyPost.co.uk, Dr. Lodhi shares expert perspectives on health, lifestyle, and medical awareness to help readers live healthier, more balanced lives.


