7 Powerful Facts About Dorsalgia: Meaning, Causes & Treatment Explained
Back pain can feel confusing and even frightening, especially when a report suddenly mentions dorsalgia. You may wonder if it is serious, permanent, or even dangerous.
Dorsalgia is simply a medical term for back pain that affects the muscles, ligaments, bones, or discs of your spine. It can appear in your neck, mid-back, or lower back. It may feel sharp, dull, burning, or achy.
Up to 40% of people over 40 live with some form of back pain. It is one of the top reasons for doctor visits worldwide and a major cause of disability. You are not alone, and importantly, many cases improve with the right care. 💙
Let’s walk through 7 powerful facts that explain dorsalgia meaning, causes, treatment options, and how you can protect your spine.
1. Dorsalgia Meaning: What Is Dorsalgia, Exactly?
Many people ask, what is dorsalgia when they first see it on a scan report.
In simple terms, dorsalgia meaning is:
- “Dorsal” = related to the back
- “-algia” = pain
So, dorsalgia describes back pain in general. It does not, by itself, explain the exact cause. Instead, it tells you the location of your pain: somewhere along your spine.
Acute vs. Chronic Dorsalgia
Dorsalgia can be:
- Acute
- Lasts less than 6–12 weeks
- Often linked to a strain, sprain, or minor injury
- Chronic
- Lasts longer than 3 months
- May involve disc degeneration, arthritis, or structural issues
A short episode after heavy lifting is often acute. Ongoing lower back pain that keeps returning may be chronic.
Why Doctors Use the Term “Dorsalgia”
Doctors use this term because:
- It is neutral and descriptive
- It allows for more details later
- It avoids guessing the cause too early
From there, they may add more information. For example, they may mention disc problems, arthritis, or nerve compression once tests are complete.
🧠 Real-life example:
Sara, 45, sees “lumbar dorsalgia” on her MRI report. Her doctor explains it means “lower back pain,” then orders therapy and posture changes rather than immediate surgery.
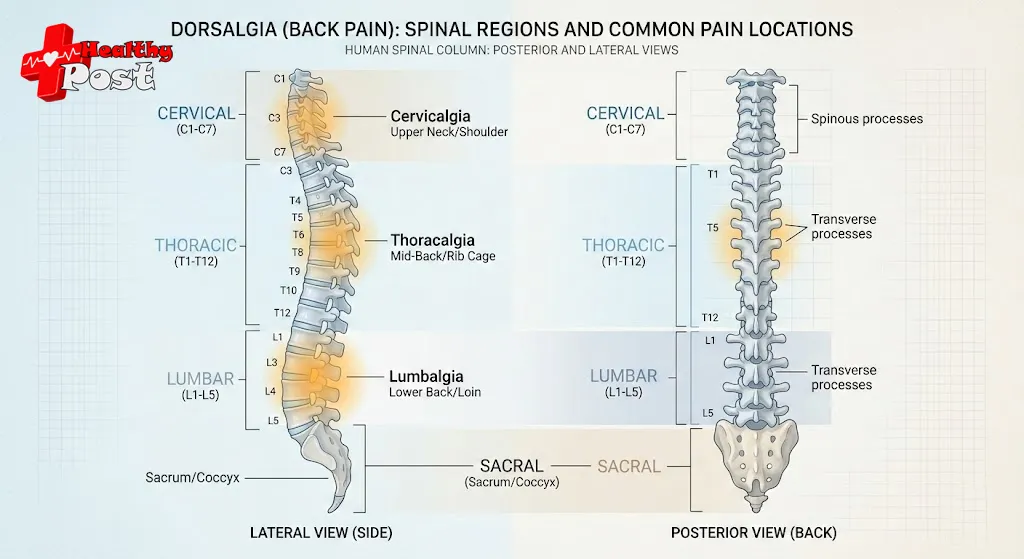
2. Fact 2: The Types of Dorsalgia Depend on Where It Hurts
Your spine has several regions. Doctors classify back pain based on which part hurts. This helps guide diagnosis and treatment.
Main Types of Dorsalgia by Spinal Region
| Type of dorsalgia | Spine region involved | Common area of pain | Typical triggers |
|---|---|---|---|
| Cervical dorsalgia | Neck | Neck, shoulders, upper back | Screen time, whiplash, poor posture |
| Cervicothoracic | Neck + upper back | Base of neck, between shoulders | Forward head posture, heavy bags |
| Thoracic dorsalgia | Mid-back | Between shoulder blades | Slouching, twisting, muscle strain |
| Thoracolumbar | Mid-back + lower back | Mid to low back area | Lifting, rotation, falls |
| Lumbar dorsalgia | Lower back | Belt line area or just above | Bending, lifting, sitting long hours |
| Lumbosacral dorsalgia | Lower back + sacrum | Lower back, tailbone, buttocks | Disc issues, arthritis, pregnancy strain |
How Each Region May Feel
- Neck (cervical)
- Stiffness, headaches, pain with head turning
- Mid-back (thoracic)
- Pain after long sitting, twisting, or poor posture
- Lower back (lumbar and lumbosacral)
- Aching, sharp twinges, or pain shooting into hips or legs
Knowing the region helps you describe your pain more clearly. This improves your doctor’s ability to tailor treatment.
🧠 Real-life example:
A desk worker feels burning pain between the shoulder blades after long computer sessions. This often fits thoracic dorsalgia linked to posture.
3. Fact 3: Everyday Habits Are Major Causes of Back Pain 😮
Many causes of back pain are not dramatic injuries. They come from everyday strain on the spine.
Common Causes of Dorsalgia
- Muscle strain or ligament sprain
- Improper lifting
- Sudden twisting or bending
- Overexertion during exercise or work
- Poor posture and ergonomics
- Slouching at a desk
- Leaning forward toward screens
- Workstations set too high or too low
- Herniated discs
- The disc’s soft center pushes out
- Can press on nearby nerves
- May cause radiating pain or numbness
- Degenerative disc disease
- Age-related disc wear and dehydration
- Discs lose height and cushioning
- Can cause stiffness, aching, and reduced flexibility
- Osteoarthritis of the spine
- Cartilage in facet joints breaks down
- Bones rub and form spurs
- Pain often worse with activity, better with rest
- Traumatic injuries
- Falls or car accidents
- Sports injuries
- Heavy impact to the spine
- Other contributing factors
- Obesity, which increases spinal load
- Sedentary lifestyle and weak core muscles
- Smoking, which reduces disc blood flow
- Stress, which tightens muscles
- Conditions like scoliosis or spinal stenosis
Back Pain Is Extremely Common Worldwide
The World Health Organization back pain fact sheet notes that low back pain is a leading cause of disability across the globe. This highlights how widespread dorsalgia is, and why early care matters.
People often blame one sudden movement. In reality, pain may reflect months or years of small stresses on the spine.
4. Fact 4: Symptoms Range from Local Ache to Radiating Nerve Pain
Dorsalgia can appear in many ways. Some signs are mild and short-lived. Others signal more serious conditions.
Typical Symptoms of Dorsalgia
- Localized back pain
- Dull, sharp, burning, or throbbing
- Pain may worsen with certain movements
- Radiating pain
- Spreading into hips, buttocks, or legs
- Sometimes called sciatica when it follows the sciatic nerve
- Muscle stiffness or spasms
- Tight, knotted muscles
- Difficulty straightening up
- Limited range of motion
- Trouble bending, twisting, or turning the neck
- Numbness, tingling, or weakness
- In arms or legs when nerves are compressed
Red-Flag Symptoms: When to Seek Urgent Care 🚨
Get urgent medical help if you notice:
- Loss of bladder or bowel control
- Severe weakness in legs or arms
- Sudden, intense back pain after trauma
- Fever, chills, and back pain together
- Unexplained weight loss with ongoing pain
These signs may point to serious conditions. Examples include nerve root compression, infection, or even fractures.
The Mayo Clinic overview of back pain emphasizes that while most back pain improves with conservative care, red-flag symptoms should never be ignored.
🧠 Real-life example:
John, 52, has long-standing lower back pain. One day, he develops leg weakness and numbness. His doctor sends him for emergency imaging to rule out severe nerve compression.

5. Fact 5: Diagnosis Goes Beyond “Dorsalgia Unspecified”
You might see the phrase dorsalgia unspecified on a medical report. This usually means:
- The presence of back pain is clear
- The exact underlying cause is not fully defined yet
- More details may come after further evaluation
It does not automatically mean something is being missed. It just reflects the early stage of investigation.
How Doctors Diagnose Back Pain
- Medical history
- When did the pain start?
- What makes it better or worse?
- Any injuries, sports, or heavy lifting?
- Physical examination
- Check posture and spinal alignment
- Test range of motion
- Evaluate muscle strength and reflexes
- Look for areas of tenderness or spasm
- Imaging tests
- X-rays to check bone alignment, fractures, or arthritis
- MRI to see discs, nerves, and soft tissues
- CT scans if detailed bone images are needed
- Nerve-related tests
- EMG (electromyography) to assess muscle and nerve function
- Nerve conduction studies to track how signals travel along nerves
Doctors combine these findings. Then they refine the diagnosis beyond “unspecified” when possible.
Why a Clear Diagnosis Matters
A specific diagnosis helps to:
- Choose the safest treatment
- Decide between therapy, injections, or surgery
- Plan long-term prevention
🧠 Real-life example:
A patient’s initial note says “dorsalgia unspecified.” After MRI, the doctor finds a small herniated disc pressing on a nerve. The care plan shifts to targeted physical therapy and pain management.
6. Fact 6: Treatment Options Range from Rest to Advanced Surgery 🏥
Many people fear that dorsalgia always leads to surgery. This is rarely the case. Most back pain improves with conservative treatment and time.
Conservative (Non-Surgical) Treatments
- Medications
- Over-the-counter pain relievers like paracetamol or NSAIDs
- Occasional use of muscle relaxants when needed
- Physical therapy
- Targeted stretching and strengthening
- Core stability exercises
- Posture retraining and movement education
- Chiropractic care or osteopathic manipulation
- Gentle spinal adjustments in appropriate cases
- Always check with your doctor first
- Massage therapy
- Eases tension in tight muscles
- Helps circulation and relaxation
- Pain management injections
- Corticosteroid injections to reduce inflammation
- Nerve blocks to interrupt pain signals
Lifestyle changes, which we will cover later, also play a key role in lasting results.
When Surgery Becomes an Option
Surgery is usually considered when:
- Conservative care has failed
- Symptoms severely affect daily life
- There is nerve compression with weakness or serious pain
Common surgical options include:
- Microdiscectomy
- Removes the part of a herniated disc pressing on a nerve
- Often used for leg-dominant pain from disc issues
- Electrical stimulation
- Spinal cord stimulators can block pain signals
- Typically used for chronic, difficult-to-treat pain
- Spinal fusion
- Joins two or more vertebrae
- Reduces painful motion in damaged segments
- Artificial disc replacement
- Removes a damaged disc
- Replaces it with a device that preserves motion
The Royal Spine Surgery Approach: Personalized, Modern Care
Some centers, such as a Royal Spine Surgery Approach, focus on:
- Advanced diagnostics
- High-quality MRI, CT scans, and nerve studies
- Detailed mapping of pain sources
- Multidisciplinary care
- Neurosurgeons, orthopedic spine surgeons
- Pain specialists and physical therapists
- Coordinated plans instead of isolated opinions
- Minimally invasive surgery
- Microtube spine surgery through small incisions
- Less muscle damage and often faster recovery
- Patient-centered care
- Tailored treatment plans
- Education on expectations and self-care
This style of care aims to reduce pain while protecting function and quality of life.
🧠 Real-life example:
After months of leg pain and failed therapy, a patient undergoes a microdiscectomy with a minimally invasive technique. She walks the next day and returns to light work in a few weeks, with guided rehab.

7. Fact 7: Prevention and Lifestyle Changes Can Be Powerful 💪
Even if you already have back pain, lifestyle changes can reduce symptoms and prevent flare-ups.
Posture and Ergonomics
- Sit with feet flat and knees at hip level
- Keep screens at eye level
- Use a chair with adequate lumbar support
- Take short standing or walking breaks every 30–60 minutes
Consider reading a reliable guideline on desk ergonomics and back care from trusted health organizations when setting up your workspace.
Exercise and Movement
Regular movement keeps your spine strong and flexible:
- Core strengthening
- Planks, bridges, and gentle abdominal work
- Supports the spine from the front and back
- Low-impact aerobic exercise
- Walking, swimming, or cycling
- Improves circulation and weight control
- Flexibility and balance
- Yoga or Pilates with a trained instructor
- Focus on safe form rather than extreme poses
Always start slowly and increase activity with guidance if you already have pain.
Safer Lifting Techniques
- Bend your knees, not your waist
- Keep the object close to your body
- Avoid twisting while lifting
- Ask for help with heavy or awkward loads
Quit Smoking and Maintain a Healthy Weight
- Smoking reduces blood flow to spinal discs
- This can speed up disc degeneration
- Extra weight puts pressure on the lower back
Even small weight loss and smoking reduction can translate into noticeable relief for many people.
Stress Management and Sleep
- Stress can tighten muscles and worsen pain perception
- Techniques like deep breathing, mindfulness, or counseling can help
- A supportive mattress and comfortable sleep posture can also reduce strain
🧠 Real-life example:
After adding daily walks, a brief core routine, and a better chair at work, a 38-year-old office worker reports fewer mid-back flare-ups and less stiffness in the morning.

FAQs About Dorsalgia
1. Is dorsalgia the same as a slipped disc?
No. Dorsalgia means back pain, not a specific cause. A “slipped” or herniated disc is one possible cause of that pain. Imaging helps clarify whether a disc is involved.
2. Is dorsalgia unspecified something to worry about?
Not automatically. Dorsalgia unspecified usually means back pain is present, but the exact cause is not yet defined. It often appears on early reports. Your doctor may request more tests or follow-up if needed.
3. Can dorsalgia be cured?
Many people experience complete relief, especially from acute episodes. Chronic back pain can often be managed with therapy, lifestyle changes, and, in some cases, procedures or surgery. The aim is to reduce pain and improve function.
4. When should I see a doctor for back pain?
See a doctor if back pain:
- Lasts longer than a few weeks
- Keeps returning
- Radiates into your arms or legs
- Comes with numbness, tingling, or weakness
Seek urgent care if you have red-flag symptoms like fever, trauma, or bladder or bowel changes.
5. Can exercise make dorsalgia worse?
The wrong exercises can aggravate pain, especially if too intense or done with poor form. However, appropriate, guided exercise usually helps. A physical therapist can design a safe program tailored to your condition.
6. Do I always need an MRI for back pain?
No. Many cases improve with conservative care without advanced imaging. MRI or CT is used when red-flag symptoms, severe pain, or suspected structural issues are present. Your doctor decides based on your history and exam.
Conclusion: Taking Charge of Dorsalgia and Your Spine Health 🌱
Understanding dorsalgia removes much of the fear around that unfamiliar word. It means back pain that can involve muscles, ligaments, discs, or joints in your spine. It may be localized or radiating, mild or intense, acute or chronic.
You have learned:
- The dorsalgia meaning and its different regional types
- Common causes, from muscle strain to disc disease and arthritis
- How symptoms guide diagnosis and when red flags matter
- Why “dorsalgia unspecified” is often just an early label
- The spectrum of treatments, from gentle therapy to modern minimally invasive surgery
- The impact of posture, exercise, weight, smoking, and stress
Back pain is common, but you are not powerless. With informed medical care, consistent self-care, and, when needed, specialist support, many people regain comfort and confidence in their daily lives.
If you are living with back pain now, consider speaking with a spine-aware doctor or a multidisciplinary clinic. Ask questions, share your goals, and explore a plan tailored to you. Your spine carries you through life; it deserves thoughtful attention and care. 💙


One thought on “7 Powerful Facts About Dorsalgia: Meaning, Causes & Treatment Explained”