8 Easy Steps on How to Collect a Sputum Culture Test Safely
Worrying about a lung infection can be stressful 😟. Tests and medical terms may feel confusing or even scary.
A sputum culture test is one of the most important tools doctors use to understand what is happening in your lungs. It helps them find the exact germ causing your symptoms, so they can choose the right treatment.
This guide walks you through 8 easy, safe steps on how to collect sputum culture samples correctly. You will learn what the test is, how to prepare, what your sputum color can mean, and how to understand your results.
1. Understand What a Sputum Culture Is and Why It Matters 🫁
Before you learn sputum culture how to collect, it helps to know exactly what the test does.
What is a sputum culture?
You may wonder, what is a sputum culture and how is it different from a throat swab.
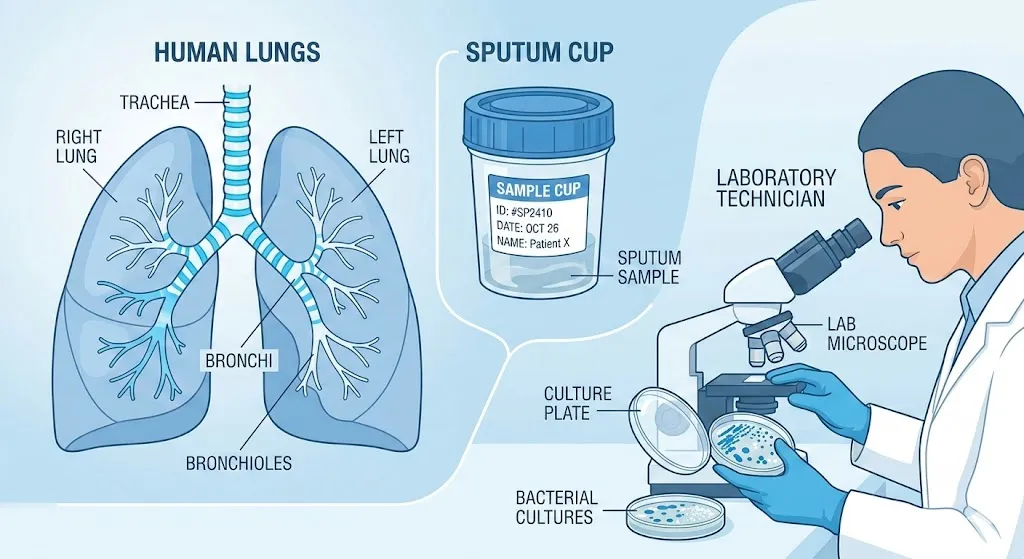
- Sputum is thick mucus (phlegm) from deep in your lungs and airways.
- It is not the same as saliva. Saliva comes from your mouth and is much thinner.
- Sputum contains immune cells, bacteria, and sometimes fungi from your lower airways.
In a sputum culture, the lab places your sputum on special plates that help germs grow. Then they:
- Watch which bacteria or fungi grow.
- Test which antibiotics or antifungals can kill those germs.
You might see your doctor write “sputum = phlegm.” Both words refer to mucus from the respiratory tract.
To learn more, medical sites like MedlinePlus explain sputum culture in simple language.
Why doctors order this test
A sputum culture helps your provider:
- Diagnose bacterial or fungal infections in the lungs and airways.
- Identify conditions like:
- Pneumonia
- Tuberculosis (TB)
- Bronchitis and bronchiectasis
- Infections in cystic fibrosis
- Monitor chronic lung diseases, such as COPD or cystic fibrosis.
- Check whether your treatment is working or needs adjustment.
- Decide if you need more tests, such as imaging or blood tests.
Often, the lab also does a Gram stain. This quick test shows whether bacteria are Gram-positive or Gram-negative. That helps guide early antibiotic choices while the full culture is still growing.
Understanding this first step can make your sputum culture test feel less mysterious and more manageable.
2. Notice What Your Sputum Looks Like 👀
Paying attention to color, thickness, and amount of sputum can give useful clues. It does not replace medical testing, but it can help you describe your symptoms better.
Common sputum colors and what they may mean
Here is a quick overview of sputum color and possible causes:
| Sputum Color | What It May Suggest | When to Call a Doctor |
|---|---|---|
| Clear | Often normal. Large amounts may suggest lung disease or irritation. | If it is persistent or you have breathing symptoms. |
| White/Gray | May be normal. Large amounts can appear with chronic lung disease. | If it increases, or with cough, wheezing, or chest discomfort. |
| Yellow/Green | Often bacterial infection like pneumonia or bronchitis. Common in cystic fibrosis. | Within 24 hours, especially with fever or shortness of breath. |
| Black | Seen in smokers or coal dust exposure (“black lung”). | If you smoke or work with dust, discuss screening. |
| Brown/Brown spots | May show old blood, bacterial pneumonia, bronchitis, or dust/toxin exposure. | Soon, especially if you feel unwell or it continues. |
| Pink, frothy | Can point to pulmonary edema, often linked to heart failure. | Same day or emergency care if breathing is hard. |
| Red or bright bloody | Possible lung cancer, pulmonary embolism, or major bleeding. | Emergency care immediately. Do not wait. |
Red or blood-streaked sputum, especially if new or heavy, needs urgent attention. Call emergency services or go to the nearest emergency department.
Noticing these details helps your provider interpret your sputum culture results more accurately.
3. Know When a Sputum Culture May Be Needed
You might be asked to do this test at home or in a clinic. Understanding when doctors order it can ease concerns.
Common symptoms that trigger testing
Providers may request a culture if you have:
- A persistent cough that brings up mucus or phlegm.
- Fever and chills, especially with cough.
- Shortness of breath, even at rest or with light activity.
- Chest pain, worse with deep breaths or coughing.
- Fatigue or feeling unusually weak.
- Confusion, especially in older adults, which can signal serious infection.
Sometimes, a chest X‑ray or CT scan shows signs of infection. In that case, the doctor may order a sputum test even if your symptoms are mild.
If you have chronic lung disease, like COPD or bronchiectasis, your team may use regular sputum cultures to:
- Watch for flare‑ups.
- Catch resistant bacteria early.
- Adjust inhaled or oral medications.
4. Prepare the Day Before Your Test 📝
Good preparation makes sample collection safer and more successful. That is a key part of how to collect sputum culture samples correctly.
Timing and food
Most providers prefer samples first thing in the morning. Your lungs collect mucus overnight, so more sputum is ready to cough up.
The day and night before:
- Drink more water (unless you have fluid limits). This helps thin the mucus.
- Avoid heavy meals late at night.
- Do not eat for 1–2 hours before the test, if your provider advises this.
If a bronchoscopy is planned, you may need to fast up to 12 hours. Follow the exact instructions from your care team.
Medications
Tell your provider about:
- All prescription and over‑the‑counter medicines.
- Inhalers, nebulizers, and nasal sprays.
- Antibiotics you took in the last few weeks.
Antibiotics can change culture results. Your doctor might delay the test or adjust treatment based on this.
Never stop antibiotics on your own without medical advice.
5. Get Ready Right Before Collection 🫧
The moments just before sample collection matter more than many people realize. This step helps avoid mixing saliva with sputum.
Clean, but not minty
Right before the test:
- Rinse your mouth with plain water. Swish and spit a few times.
- Do not brush teeth or use mouthwash right before the test, unless told.
- Avoid strong flavors like mint, which can make you swallow more.
The goal is a cleaner mouth so fewer mouth bacteria end up in the cup.
Relax and position yourself
- Sit upright in a chair or at the bedside.
- Lean slightly forward.
- Place the sterile cup where you can reach it easily.
- Keep tissues nearby.
If you feel anxious, try slow, deep breaths through your nose and out through your mouth. Stress can make coughing harder.
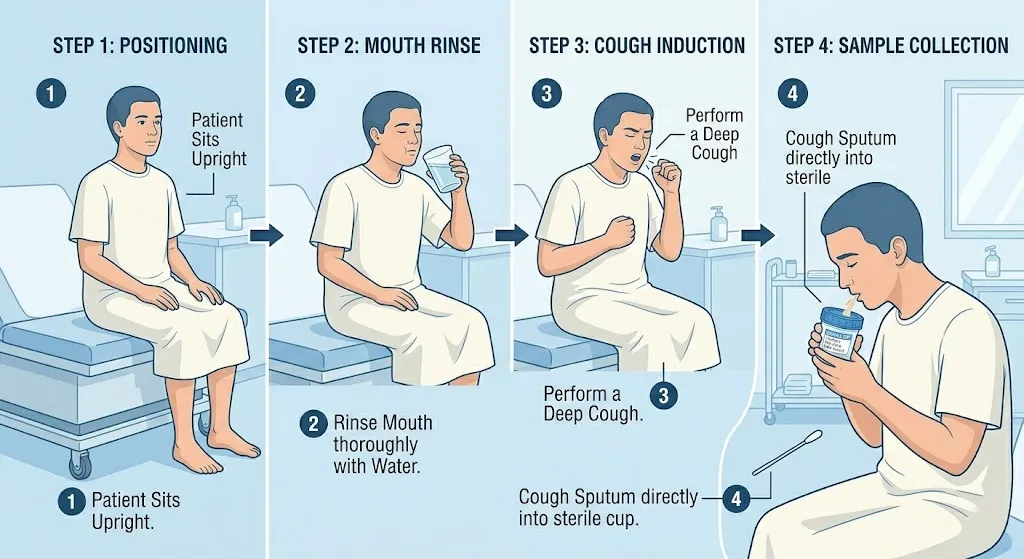
6. How to Collect Sputum Culture Safely, Step by Step ✅
This is the heart of sputum culture how to collect. These steps apply whether you are at home or in a clinic. Always follow the instructions your provider gives you, as details may vary.
Step‑by‑step collection guide
- Wash your hands
- Use soap and water or hand sanitizer.
- Dry your hands well.
- Check the container
- Make sure it is sterile and unopened.
- Look for your name and date of birth on the label, if pre‑labeled.
- Loosen the mucus
- Take several deep breaths.
- Inhale slowly through your nose.
- Exhale through your mouth.
- On the third or fourth breath, hold it a moment, then cough.
- Cough from deep in the chest
- Try to cough from deep in your lungs, not just your throat.
- It may feel like a strong “huff” from your belly.
- You can place a hand on your upper belly to feel the movement.
- Collect the sputum, not saliva
- When you feel mucus move up, bring the cup close to your mouth.
- Spit or gently “expectorate” the sputum into the cup.
- Avoid filling it with thin, clear saliva alone.
- Aim for the requested amount
- Many labs prefer about a teaspoon (5 mL) or more.
- If you are unsure, ask your provider.
- Seal and label the container
- Close the lid tightly to avoid leaks.
- Check that your name, date, and time of collection are correct.
- Wash your hands again
- Wash or sanitize your hands after handling the container.
If you have difficulty, your healthcare worker may:
- Tap gently on your chest or back to help loosen mucus.
- Ask you to inhale a salty (saline) mist to trigger coughing.
These methods are safe for most people and can improve the quality of the sample for your sputum culture test.
7. What If You Cannot Cough Up Enough Sputum?
Sometimes, even with good effort, not enough sputum comes up. Your provider still needs a lower airway sample. In that case, they may suggest a bronchoscopy.
What is bronchoscopy?
A bronchoscopy is a procedure where a doctor:
- Gently inserts a thin, flexible tube through your nose or mouth.
- Guides it down into your windpipe and lungs.
- Uses a tiny camera to see the airways.
- Collects mucus or small tissue samples.
You receive medicine to make you comfortable and possibly sleepy.
Trusted medical sources, such as Mayo Clinic, describe bronchoscopy in more detail if you want additional background.
Preparation and safety
If bronchoscopy is planned:
- You may need to fast for several hours before.
- Tell the team about all medications, especially blood thinners.
- Arrange for someone to drive you home, due to sedation.
Risks are low but can include:
- A sore throat after the procedure.
- Temporary difficulty coughing or swallowing.
- A short period where you cannot eat or drink until your cough reflex returns.
Your team will monitor you and give specific instructions. Although more involved than simple coughing, bronchoscopy can provide a very accurate sample for culture.
8. Understand Your Results and Next Steps 🧪
Once your sample reaches the lab, staff begin the sputum culture process. Results do not come back instantly.
How long results take
- Some bacteria grow in 1–3 days.
- Others are slower and need up to a week or more.
- Tuberculosis and some fungi can take several weeks.
It is normal to feel impatient, but the lab needs time to grow and correctly identify the germs.
What “normal” and “abnormal” mean
- Normal result
- No harmful bacteria or fungi grew.
- Usual mouth or upper airway bacteria may appear, but not in dangerous amounts.
- Abnormal result
- Specific bacteria or fungi grew in higher numbers.
- Common findings include germs that cause:
- Pneumonia
- Acute or chronic bronchitis
- Tuberculosis
- Infections in COPD or cystic fibrosis
Your doctor will compare results with:
- Your symptoms and physical exam.
- Imaging like X‑rays or CT scans.
- Blood tests or other lab work.
You may hear terms such as “sensitive” or “resistant.” These describe how well antibiotics work against the bacteria found. That helps guide your treatment plan.
If the infection is serious or you have other health issues, you may be referred to a lung specialist (pulmonologist) for follow‑up.
Safety, Risks, and When to Seek Urgent Help 🚨
The basic act of coughing sputum into a cup is very safe. For most people, there are no significant risks. You may cough more than usual during collection, but this should settle quickly.
Bronchoscopy, when needed, carries small risks, such as:
- Sore throat or hoarse voice.
- Mild bleeding from irritated airways.
- Temporary breathing discomfort.
Your medical team will explain these risks, monitor you, and tell you when it is safe to eat or drink again.
Call your doctor promptly if you notice:
- Worsening shortness of breath.
- High fever or chills.
- New or increasing chest pain.
- Thick yellow, green, or brown sputum that is getting worse.
Seek emergency care immediately if:
- Your sputum is red, bright, or looks like fresh blood.
- You suddenly cannot catch your breath.
- You have severe chest pain, especially with breathing.
- You feel faint, confused, or very weak.
These signs could mean a serious condition such as pulmonary embolism, major bleeding, or severe infection.
FAQs About Sputum Culture Tests ❓
1. Is a sputum culture test painful?
Collecting sputum by coughing into a cup is not usually painful. You may feel some chest tightness or irritation from coughing. Bronchoscopy may cause a sore throat later, but pain is usually mild and short‑lived.
2. Can I do the test at home?
Yes, many people collect their sample at home. You receive a sterile cup and written instructions. Follow the eight steps in this guide and return the sample to the lab as directed, usually the same morning.
3. What if I accidentally spit mostly saliva?
If the sample is mostly saliva, the lab may report that it is “contaminated” or “inadequate.” Your provider might ask you to repeat the test. Focus on deep breathing and coughing from your chest next time, not just clearing your throat.
4. Will I need more tests after a sputum culture?
It depends on your situation. Some people improve with treatment guided by the culture alone. Others may need more tests, such as chest imaging, lung function tests, or blood work. Your doctor will decide based on your results and symptoms.
5. Can this test detect lung cancer?
A sputum culture is designed to find bacteria and fungi, not cancer cells. Sometimes, separate tests on sputum or imaging studies help detect lung cancer. If you cough up blood or have other concerning signs, your provider may order additional tests.
6. How often will I need this test if I have chronic lung disease?
People with COPD, bronchiectasis, or cystic fibrosis may need sputum cultures several times a year, especially during flare‑ups. Your lung specialist will set a schedule based on your history and symptoms.
Bringing It All Together 🙌
A sputum culture test is a simple but powerful tool for understanding lung and airway infections. It helps your healthcare team:
- Discover which bacteria or fungi are present.
- Decide which treatments are most likely to work.
- Monitor chronic lung conditions, like COPD and cystic fibrosis.
By following these 8 easy steps—from understanding the test, to noticing sputum color, preparing properly, collecting the sample, and understanding results—you play an active role in your care.
If you are ever unsure about how to collect sputum culture samples, ask your nurse, doctor, or respiratory therapist to walk you through the steps again. They are there to help you feel safe and supported.
Use what you have learned here to:
- Talk confidently with your healthcare team.
- Recognize warning signs early.
- Support your lungs with timely testing and treatment.
If your provider suggests a sputum culture test, you now know what to expect, how to prepare, and how to collect a sample safely and effectively. Your effort can make a real difference in getting the right diagnosis and the right care at the right time. 🫁💙